Get Healthy You in your inbox
Check the “Healthy You” box below to to receive the latest news, health tips and stories in your email every week.
Health Tips
Health and wellness tips to help you live a healthy life
Learn the signs, symptoms and treatment options for irritable bowel syndrome in children
Stories
Patients and colleagues share their stories and experiences
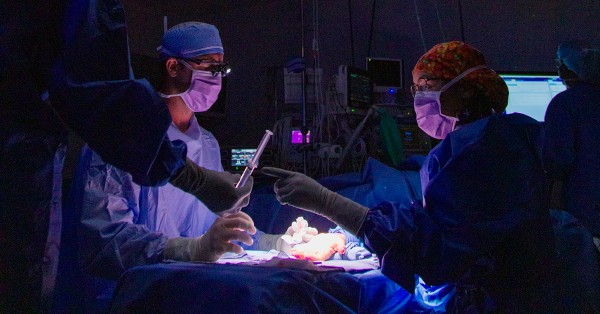
Bariatric surgery helps steer truck driver toward a happier, healthier life
COVID Care Center
How to protect yourself and your family from COVID-19 and other respiratory illnesses.
LVHN in the News
Lehigh Valley Physicians Group new building dedicated in Pine Grove, longtime doctor honored
via Pottsville Republican
April 25, 2024
Good News/Pediatric cancer survivor becomes nurse, works with LVHN nurse who cared for her
via WFMZ-TV 69 News
April 25, 2024
‘In every community law enforcement is fighting’: Drug take-back day takes aim at prescription medication abuse
via LehighValleyNews.com
April 24, 2024
Pocono Family YMCA expansion set to break ground by end of summer
via Pocono Record
April 22, 2024